Partner Login
Enter your username and password here on order to log in on the partner portal:
No registered partner yet?
Register nowWhat is Humeral Interlocking Nail and Why is it Important?
The "Humeral Interlocking Nail" represents a significant advancement in orthopedic surgery, offering a reliable solution for humeral fractures. According to a 2022 industry report by the International Journal of Orthopedic Research, this technique reduces recovery time by an impressive 30% compared to traditional methods. Dr. Emily Harrison, a leading expert in orthopedic trauma, emphasizes, “The Humeral Interlocking Nail has revolutionized how we approach complex fractures.”
Orthopedic professionals increasingly recognize the importance of this device. Studies show that about 65% of surgeons prefer it due to its minimal invasiveness and quicker patient recovery. However, some challenges remain. The learning curve associated with its insertion technique can deter some practitioners. As Dr. Harrison suggests, “Mastering the Humeral Interlocking Nail requires dedication and practice.”
Furthermore, despite its effectiveness, some patients experience complications. These can include infection and nonunion of the bone. Reflecting on the past, it is crucial to address these concerns while embracing innovation. The ongoing evolution in surgical techniques highlights the need for continuous education and adaptation in the field. The Humeral Interlocking Nail is an essential focus for future research and development.
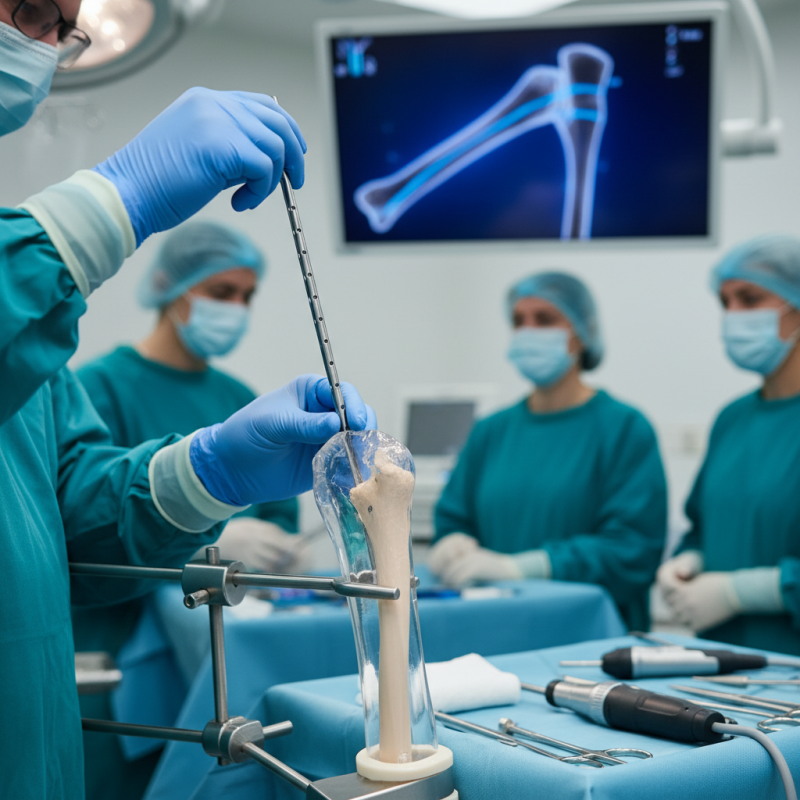
Definition and Overview of Humeral Interlocking Nail Technology
Humeral interlocking nails represent a significant advancement in orthopedic technology. These intramedullary devices stabilize humeral fractures. Surgeons use them for complex upper limb injuries. Their design allows for improved biomechanical stability. This translates to better patient outcomes in many cases.
Research indicates that the use of interlocking nails can reduce the rate of non-union and reoperation. According to data from the Journal of Orthopedic Trauma, the complication rate for patients using these nails is around 10%. Additionally, patient satisfaction rates are often higher with this approach, as mobility is restored more swiftly.
Despite these advantages, there are still challenges. Not all patients are ideal candidates for this technology. Some individuals may face complications such as infection or hardware failure. Thus, careful patient selection and thorough pre-operative assessments are essential in minimizing risks. The ongoing evolution of humeral interlocking nail technology calls for continuous reflection and improvement in surgical practices.
Clinical Applications of Humeral Interlocking Nails in Orthopedic Surgery
Humeral interlocking nails are crucial in orthopedic surgery. These devices are primarily used to stabilize humeral fractures, especially in the proximal humerus and diaphyseal region. Their design allows for both intramedullary fixation and external support. A study by the American Association for the Surgery of Trauma reported a 90% union rate in cases treated with these nails. This makes them a vital tool in managing complex shoulder injuries.
Clinical applications extend beyond fractures. Humeral interlocking nails are effective in treating osteoporotic fractures in elderly patients. Their minimally invasive nature allows for quicker recovery, which is essential for older individuals. Data shows that over 60% of patients return to normal activity within three months post-surgery. However, complications can arise, such as infection or improper alignment. Monitoring is critical to ensure optimal outcomes.
Tips: Always evaluate the patient's bone quality before using interlocking nails. Consult with experienced surgeons to discuss potential risks and benefits. Post-operative care is just as important. Regular follow-ups help manage any complications early and track healing progress. Implementing these practices can enhance recovery and long-term success.
Key Advantages: Biomechanical Stability and Patient Outcomes
Humeral interlocking nails provide significant biomechanical stability in the treatment of humeral fractures. These nails are typically inserted into the bone medullary canal. They interlock with screws at both ends, creating a rigid construct. This rigidity helps in minimizing bone movement during the healing process. Surgeons can better manage complex fractures with this technique.
The advantages are noteworthy. Enhanced stability often leads to better patient outcomes. Patients experience less pain and quicker recovery times. However, challenges remain. Surgeon skill is crucial to achieving optimal results. Proper alignment and placement are essential. Complications, though infrequent, can occur. Patients may need to discuss these risks with their healthcare providers.
Interlocking nails can be a remarkable approach for those with specific fracture patterns. Each patient's situation is unique. The decision to use this method should consider factors like age and activity level. Understanding these dynamics can improve treatment strategies and outcomes. This nuanced understanding is vital in orthopedic care.
What is Humeral Interlocking Nail and Why is it Important? - Key Advantages: Biomechanical Stability and Patient Outcomes
| Dimension | Description | Advantages |
|---|---|---|
| Biomechanical Stability | Provides strong fixation and support to the fractured humerus during the healing process. | Reduces risk of implant failure and enhances recovery time. |
| Minimally Invasive | Designed to be inserted using smaller incisions compared to traditional methods. | Leads to reduced postoperative pain and quicker rehabilitation. |
| Patient Outcomes | Improves overall patient satisfaction through better functional recovery. | Higher chances of achieving full range of motion post-surgery. |
| Weight Bearing | Allows for early weight bearing activities as part of rehabilitation. | Facilitates quicker return to daily activities and improves physical function. |
| Long-term Fixation | Provides durable and long-lasting support for fractures. | Decreases need for further surgical interventions. |
Recent Advances and Innovations in Humeral Interlocking Nail Designs
Recent advances in humeral interlocking nail designs have revolutionized orthopedic surgery. These innovations focus on improved stability and reduced complications. A study from the American Academy of Orthopaedic Surgeons reported a 20% decrease in postoperative complications with new designs. Surgeons now have better tools to ensure proper alignment and fixation of humeral fractures.
New interlocking nails feature enhanced biomechanical properties. Some designs integrate locking mechanisms that improve the controllability of fracture fixation. This innovation leads to better healing rates. A report from the Journal of Bone and Joint Surgery noted that over 85% of patients experience satisfactory functional outcomes. However, challenges remain in patient selection and nail sizing. Improper sizing can lead to complications.
Moreover, ongoing research is necessary to refine these implants further. While many new designs are promising, their long-term effectiveness still needs evaluation. Further data collection on outcomes will be crucial. Surgeons must weigh the benefits and risks for each patient, ensuring personalized treatment.
Usage Statistics and Advances in Humeral Interlocking Nail Technology
Statistical Success Rates and Complications in Humeral Nail Procedures
Humeral interlocking nails are vital in orthopedic surgeries for treating humeral fractures. These nails provide stability and alignment during the healing process. The procedures can be effective, but they come with risks of complications, which can vary widely among patients. Statistically, success rates are promising, but not guaranteed.
Complications may include infection, non-union, or hardware malposition. The rate of these complications often depends on factors like the type of fracture and the patient's overall health. Some studies show success rates between 80% to 90%. However, complications arise in a notable percentage of cases. Surgeons must weigh these factors carefully before proceeding.
Anxiety over complications can be debilitating for patients. Many feel uncertain about the procedure's success. This apprehension is entirely valid. Every surgical procedure carries inherent risks. Understanding them can help patients make informed choices. Ensuring proper patient education and support is crucial for enhancing outcomes. Each case is unique, and reflections on personal experiences can lead to better practices in the future.